If your dental professional suspects problems with your TMJ, they have a number of ways to determine whether your jaws and protective cartilage discs are in the correct position.
A medical and dental history along with an examination of the teeth and the dental arches
Patients are asked questions regarding possible symptoms of TM dysfunction. If the patient answers “yes” to any of the symptoms (including headaches, earaches, ringing in the ears, sore neck, dizziness or fainting), and “yes” to clenching and bruxing, further tests are usually performed.
Patients are examined for how wide they can open the jaw and move it to the left, right and forward, and whether the jaw opens straight or moves in either direction. Structural issues inside the jaw can lead to issues with achieving a normal range of motion.
If a patient clenches and grinds their teeth at night, their head and neck muscles will likely be extremely sore. It’s a common symptom of TMD issues and, if there’s a decrease in pain over time, an indicator that treatment is working if there’s a decrease.
TMJ X-Rays (tomogram x-rays) can help reveal whether the lower jaw bone, called the condyle, is too far back on either side when the patient bites down on the back teeth. When this happens, it can impinge on the nerves and blood vessels at the back of the socket.
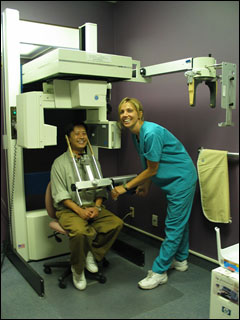
Tomogram X-Ray Machine
When the joints of the body are functioning normally, there should be no noise or vibrations. A Computerized Joint Vibration Analysis, of JVA, uses specialized equipment to take readings of any noises or vibrations that occur when the jaw is opened or closed. It’s a simple, noninvasive test that only takes a few minutes and works by placing headphones on the jaw joints while the patient opens and closes. An abnormal or dislocated joint has distinctive vibrations that can be analyzed to help diagnose the seriousness of the problem.
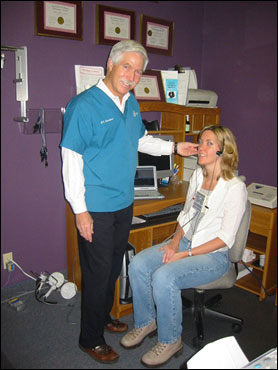
Joint Vibration Analysis Test
Our office has the knowledge and experience needed for proper, thorough diagnosis and treatment of temporomandibular joint dysfunction.
In TMD, disc displacement happens in five stages. Ideally, treatment should begin in Stage 1 or Stage 2 for ideal results. Treatments can also vary depending on the symptoms and severity, but typically involves several phases.
The immediate goal is to relieve any muscle spasms and pain and establish normal range of motion of the lower jaw. This often involves a temporary device that’s worn over the teeth. Once the pain is stabilized, your dentist will work to correct the way the teeth fit together. Permanent correction may involve selective dental treatments such as reshaping of the teeth, building crowns on the teeth, orthodontics or a permanent appliance to cover the teeth. If the jaw joint itself is damaged, however, it must be specifically treated.
Although rare, surgery is sometimes required to correct a damaged joint. However, conservative and nonsurgical treatment options are always explored first.
To solve the problem of forward head posture which can cause cervical (neck) problems, referral to a dentist or orthodontic clinician who uses functional jaw orthopedic appliances should be made. These appliances such as the Twin Block, MARA or Herbst Appliance successfully reposition the lower jaw forward and eliminate the forward head posture.
For patients who are experiencing clicking or popping sounds, a lower orthotic can be worn over the back teeth all day, including during meals. It’s custom made with grooves that redirect the patient’s bite into a better position that eliminates the sounds. Over time, the splint should help move the lower jaw forward and cause the cartilage disc to return to its correct position.
Patients who clench their jaws or grind their teeth at night, a nighttime splint may help relieve the associated pain in the muscles of the head and neck. This type of splint only comes in contact with the lower four front teeth, preventing the back teeth from touching. This can not only prevent clenching and grinding, but also morning headaches.
Once the jaw has been stabilized by a splint, one permanent solution is clear braces, which work to gradually close the space between the back teeth without discomfort. The braces may also use elastics or rubber bands to help move the teeth into the correct position, and once treatment is completed many patients report being pain-free. Patients usually wear clear braces for around 12 to 18 months.
If, after using a day or night splint, the space between the back teeth is very small, patients may want to consider crowns on the lower teeth to fill the gap. This is also a viable option if the patient has extremely large fillings or missing teeth on the lower arch.
For patients who wear dentures, a rework of either a full or partial set can help keep the jaw aligned once it is in the correct position.
Grinding at night, or bruxism, is a very common habit. Signs of bruxism include wear on the front and back teeth and defects along the gum line, also known as abfractions. A special appliance worn at night can help prevent teeth grinding.
If the teeth are misaligned, biting down can cause muscle spasms, headaches, earaches and other painful symptoms. A jaw that moves side to side or forward when biting can cause the same symptoms. For patients who are experiencing this type of pain, a bite adjustment can help correct the problem.
As part of a TMD assessment, your dentist may also do an exam to determine whether or not your shoulders, pelvis and hips are level. This can involve photos for visual examination, as well as an evaluation of the forward head posture. If any issues are found, a chiropractor may be recommended to help with realignment.
This is important because forward head posture can cause neck problems. In addition to chiropractic, your dentist may recommend an orthodontic appliance to help reposition the lower jaw forward and eliminate forward head posture.

Rondeau & Associates gives you the confident smile you have always wanted!
Privacy | Disclaimer Copyright © 2024 Digital Rein | All Rights Reserved